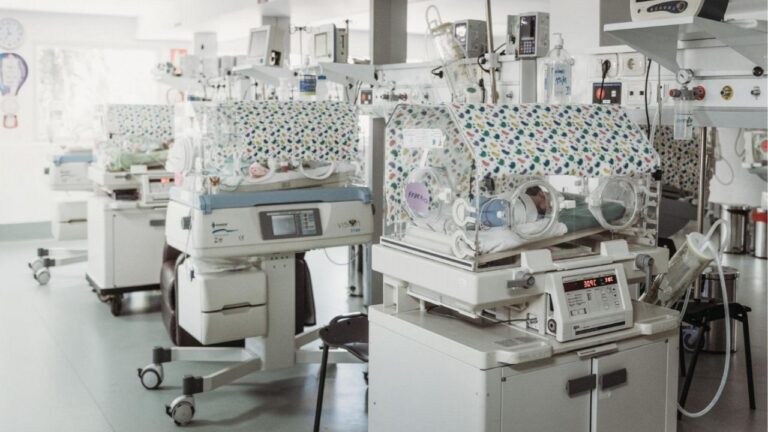
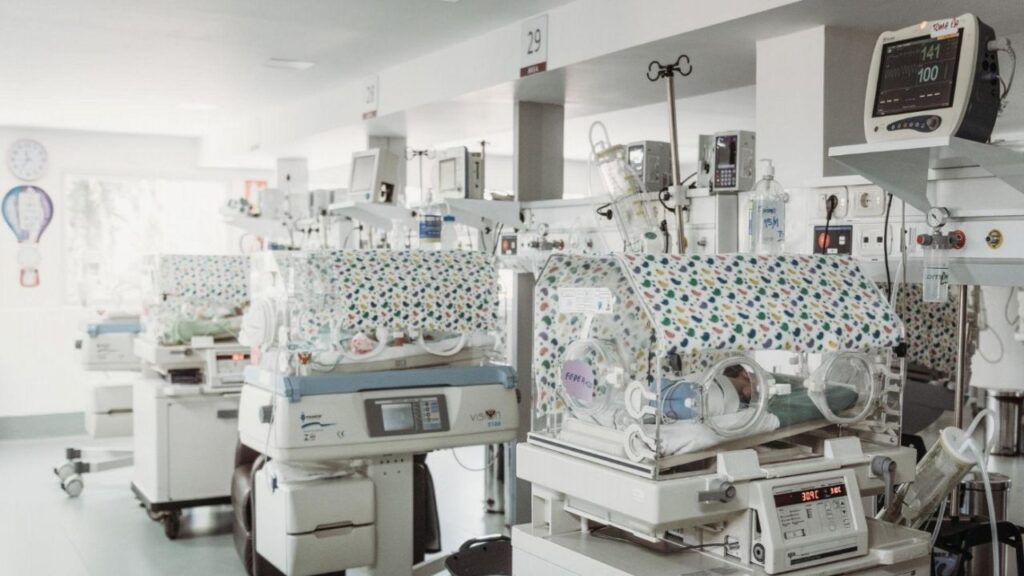
Since 2019, the team of Shiatsu Practitioners at Zen Shiatsu Uruguay has been working at the Neo-natology department of the biggest children’s hospital in Uruguay’s public health system – Hospital de la Mujer, Centro Hospitalario Pereira Rossell. In the period up until February 2020, we had given over 800 Shiatsu sessions to medical staff in their workplace, directly at the ICU and Moderate Care Units.
This strengthened our relationship with the medical team and in turn facilitated a collaboration with them and a volunteer organization, the Canguro Foundation for mothers of premature babies treated in the Intensive Care Unit. Our aim was to strengthen the mothers, so they could be physically, mentally and emotionally available for their babies and promote breast feeding. We focused specifically on the group of mothers of extreme premature babies born weighing less than 1500 grams.
In the Spotlight

Diego Sanchez
info@diego-sanchez.com
diego-sanchez.com
zenshiatsu.uy
Diego Sanchez is a pioneer of doing Shiatsu in hospitals and in emergency situations. He has been practicing and teaching Shiatsu, meditation and shamanic healing techniques for nearly 30 years.
Born and raised in Uruguay, he spent time in several European countries before moving to New York. He was there at the time of the 9-11 crisis and worked at Ground Zero and other locations giving Shiatsu to rescue workers, police and army personnel. He was also a member of the staff in Dr Oz’ integrative Medicine Program at Columbia Presbyterian Hospital, giving shiatsu to open-heart surgery and organ transplant patients in the Intensive Care Unit. Additionally, he volunteered for over 6 years at a support center for people with cancer, HIV and AIDS and at a hospice.
He now lives in Uruguay, where he organizes internationally attended retreats and directs a team of practitioners from Zen Shiatsu Uruguay, which has given nearly 2500 sessions at hospitals in the National Health System throughout the country since 2019.
Foreword
Our aim was to give support and grounding to the mothers with Zen Shiatsu, so they could relax and be confident in their bodies’ ability to produce much needed breast milk to help their babies survive through the critical post-natal period. Having the mother close with access to breast feeding is a premature baby’s best chance of survival.
Up until the moment of starting our program, the baseline was disheartening. Never in the history of this hospital, had a premature baby been nourished exclusively with a mother’s own milk. There were up to 13 different feeding indications with varied combinations that could include mother’s milk and other formulas. By the time we concluded the first year of the program, the amount of breast milk the babies had received from their own mothers had multiplied six-fold and for the first time ever, there were 4 babies who had been fed exclusively with their own mothers’ milk.
Breastfeeding and bonding between mother and baby are proven to boost survival rates of premature babies with very low weight. In this program we saw babies born weighing only 600 grams who survived!
Helping mothers and fathers to strengthen the bond with their baby, helps the whole family to handle the uncertainty of the weeks and months to come. This is crucial to improve the baby’s health until they achieve a minimum of 2,200 grams and are allowed to leave the Intensive Care Unit. However, it is a real challenge when mothers come from remote areas of the country and have to spend countless hours in the hospital corridors: they lack comfortable places to stay, they sleep very little, eat badly, are away from their other children and family and have to deal with the stress of their baby facing a high risk of dying.
We designed a special Zen Shiatsu intervention program to be implemented along with the following procedures, created by our partners, the hospital staff and Canguro Foundation volunteers:
– a new breast-feeding room that was built next to the Neo-natology Intensive Care Unit to make it easier for the mothers to be close to their babies while extracting breast milk
– improved procedures for labelling and conserving breast milk
– better coordination in delivering the mother’s milk to their babies
– improved monitoring of the welfare of those mothers, for which the shiatsu sessions were key.

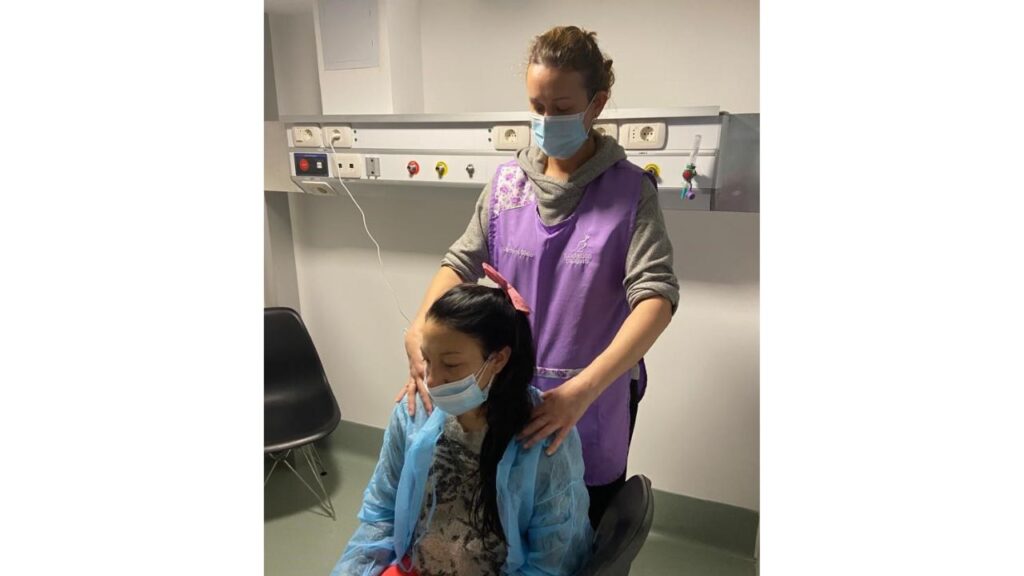

Six practitioners from the Zen Shiatsu Uruguay team are currently active in various programs. For this particular project, I designed the Shiatsu sessions and provided supervision as well as coordination with the hospital and Canguro Foundation administration. Luis Belatti and later Alice Posada visited the hospital twice a week to offer 15-minute treatments to the mothers and their partners. The sessions were conducted with the receiver sitting on a chair, and included back, shoulders, arms, hands, neck and head.
We don’t have a specific treatment room for Shiatsu. The mothers may be at different places in the hospital such as ICU, the breast-feeding room or other areas and therefore the practitioners tour the hospital looking for them and conduct the session wherever they find them. Often the mothers themselves come looking for us if they hear that we are around. Our shifts last between 2 to 4 hours, depending on the circumstances of the day.
The sessions include an accurate energetic diagnosis to focus our intention on a particular meridian function. The assessment is done each time we meet the mothers and usually includes Masunaga back zones, Yu/Shu points and energy perception techniques, all of which are performed within the first couple of minutes of each session.
Within the general routine, we focus on the specific meridian that presented in our assessment and assess the changes energetically throughout the session, to adapt to the receiver’s response. At the end, we invite them to comment on the experience, and sometimes suggest specific exercises for them to practice until our next visit.
Outcomes
From July 2020 to August 2021, we gave a total of 533 Shiatsu sessions to 168 mothers and fathers, each receiving an average of 3-4 sessions.
A data comparison run by Soledad Nuñez, head nurse of the Neo-natology department showed that:
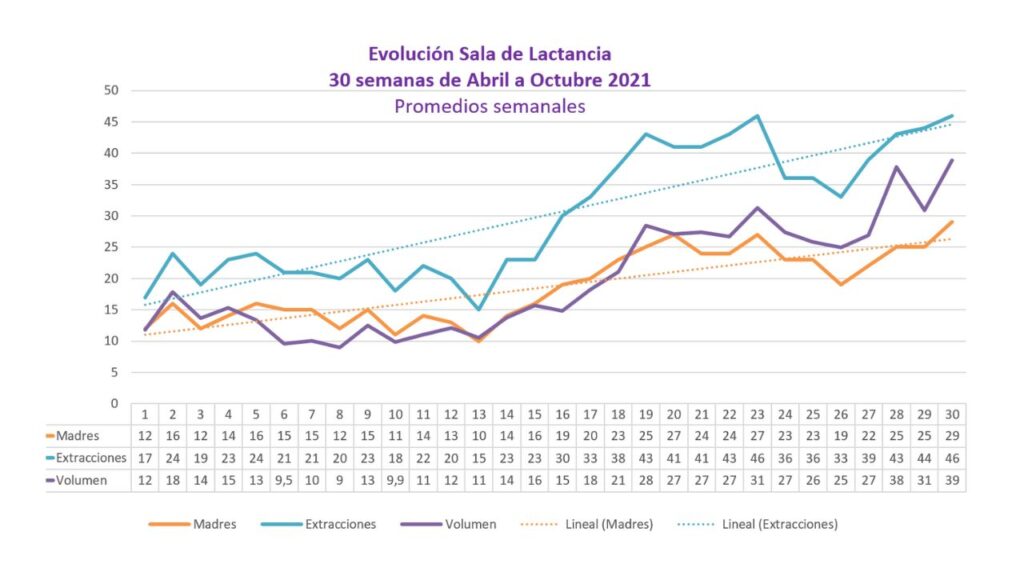
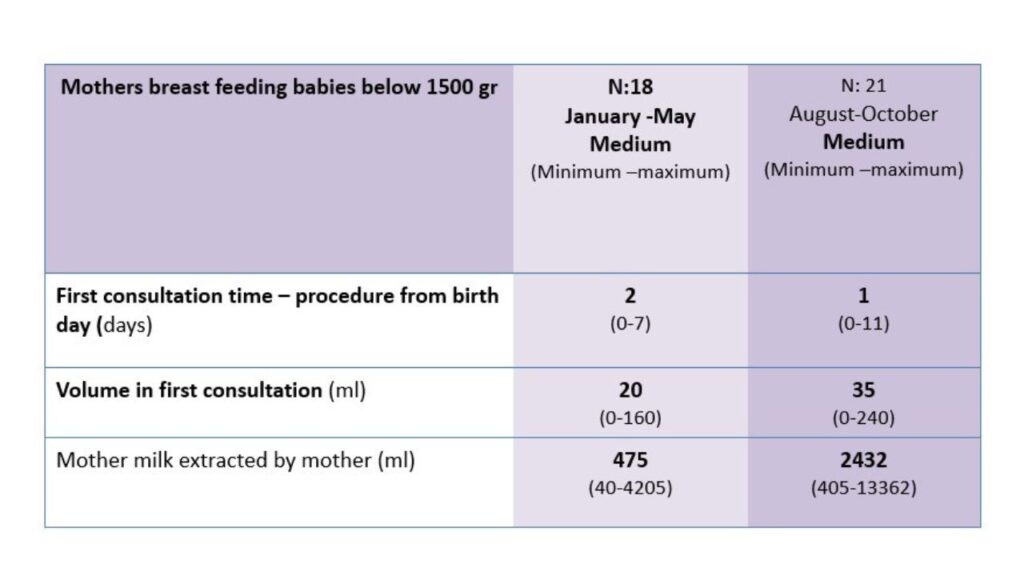
- 6.3 times more mother’s milk reached these very low weight premature babies. When the project started, the baseline mean volume was 475 ml. One year later it was 2432 ml.
- The breastfeeding period at the hospital was extended from 14 days at baseline to 34 days at the end of the study. It has been ascertained that chances of survival increase significantly after 21 days of breastfeeding.
- After one year of the program, the first consultation to start breastfeeding changed from day 2 to day 1 after birth.
- For the first time in the history of this hospital, very low weight premature babies was fed all the way from birth to discharge exclusively with their own mothers’ breast milk. From an initial 0 baseline, 4 babies were fed in this way by the end of the first year of the program.
In other studies, the implications of these improvements have been associated with better survival rates, faster weight gain, faster dismissal from critical care and possible reduction of other diseases.
Unfortunately, no means were provided in this program to measure the likely benefits in those categories but we hope they will be in the future.
The program is ongoing, with an expanded pool of volunteer Zen Shiatsu practitioners.
Our sessions are completely free of charge, both for the receivers and for the hospital. We are currently looking for financial support to create two paid positions for practitioners and fund data collection and analysis for further study proposals.
The project in figures:
| Zen Shiatsu mini-sessions | July 2021 – August2022 | % |
| Mothers | 511 | 95,87% |
| Fathers | 22 | 4,13% |
| Total | 533 | 100,00% |
Shiatsu is of great help in these situations because we can help the mother find her place, stay completely present and available for her baby, connect with herself, become whole again, discover which feelings are not useful at this moment and learn to manage them.
Alice Posada – Zen Shiatsu Team
It is part of our work to pay attention to the whole picture and consider every aspect that may become useful for the benefit of the baby’s development during their time in hospital.
Luis Belatti – Zen Shiatsu Team